Root Canal Overview
A root canal is a dental procedure that involves the extraction of root nerves from a tooth, cleaning and shaping the canal cavity and then inserting fillers to prevent bacteria from re-entering nerve system. Most often root canal is done so that the patient can retain the functional and cosmetic look. Dead nerves are considered non-vital. Even then, it’s possible for bacteria to accumulate in the nerve and cause an infection.
There are several medical reasons why one would need a root canal. Given that it’s one of the most invasive yet restorative dental. Any significant change to the tooth that disturbs or exposes the nerves can precipitate a root canal procedure, such as trauma to the tooth, this can include the following:
Dead or Dying Nerves: Dental decay, cracked teeth and dental trauma are the leading causes of dead nerves. Irreversible pulpitis caused by dental decay or deep filling can also precipitate dead nerves.
Most often the damage to the tooth is so severe that the nerve won’t be able to recover and will gradually die off. Dead or dying nerves produce some of the most painful sensations one can encounter.
Significant sensitivity: Sometimes significant levels of sensitivities can plague a tooth. Most of us have varying degrees of tooth sensitivity. However, this sensation can be so severe in some people that they can barely eat or drink cold or hot beverages and foods. Many dental interventions can be performed to alleviate this feeling. However, when all these fail root canal becomes one of the last effective resorts.
An Over Denture: Depending on the recommendation of the dentists, sometimes several roots can be preserved for the sake of preserving the supporting bone or for precision attachment. These roots upon which the denture will stay have to be filled and sealed. Exposed roots during denture can predispose the tooth to decay leading to a toothache and precipitate an tooth extraction. Ensure that only few roots that are left for this purpose to minimise the chances of future complication.
An Abscess: An abscess occurs when a tooth is too painful to chew with or use to bite down. There are two primary causes of an abscess. There is the periodontal abscess or the periapical abscess (infected tooth). Abscess of the gum tends to be different and require a different kind of treatment. However, most abscesses are treated through the removal of the affected and infected nerves through a root canal procedure.
Extensive Restorations: Sometimes the shape of the tooth has to be changed during cosmetic or medical restoration. This alteration of the shape might expose nerves and predispose them to bacteria and infection. In such a case a root canal may be the prime means of averting an infection. Alternatively, you can rely on orthodontics procedure that will preserve the tooth. This is critical especially when the dental restorations involve changes to the dental crowns and bridges.
What is the Procedure for a Root Canal?
Root canals are usually performed by a dentist or an endodontist. The study and treatment, prevention and diagnosis of ailments to the tooth nerves and dental pulp are called endodontics.
Any dentist can easily handle a typical root canal procedure. However, endodontists are best placed to perform complex root canal procedures that involve difficult tooth structures. Make sure you raise this conversation with your dentists after the initial x-ray examination. Cavity, extensive decay, and tooth fracture are the most prevalent conditions that necessitate a root canal procedure.
X-ray and Anaesthesia
The dentist starts by taking an x-ray image of the root to determine the root structure, the extent of infection and any signs of infection to the surrounding bones. After that, the dentists will inject you with local anaesthesia to numb the area around the affected tooth. If the nerve is already dead, then the dentist might not use anaesthesia. However, most dentists prefer to inject you so as to stave off any pain and discomfort you might feel during the process. The X-ray is the most critical diagnosis that informs the extent of dental work needed to be done.
Nerve Extraction
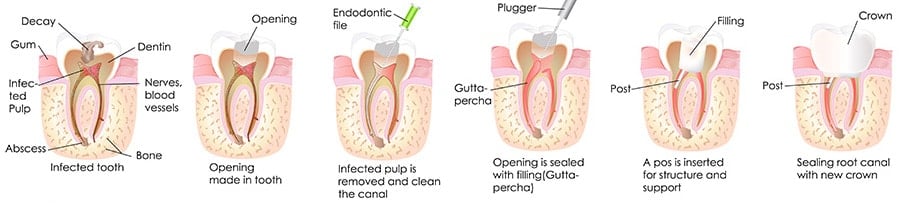
Once the anaesthesia kicks in, the dentists will then use a rubber dam around the tooth to stop the flow of saliva to the root area. When the tooth is dry, an access hole is drilled into the tooth. Decayed nerve, debris, pulp along with bacteria are pulled out through the drilled hole. Eventually, the dentist uses root canal files to clean up the area to scrub and scrape the sides of the root canal. Typically sodium hypochlorite is used as a cleaning agent for the root canal area. The anaesthesia tends to last for up to 2 hours depending on the amount used.
Root Canal Seal
Once the root canal is thoroughly cleaned, it is then permanently or temporarily sealed. Some dentists put a temporary filter that last about 5-7 days as they monitor the root canal for possible infection. There are those who prefer to seal the tooth the same day that it is drilled. Those who prefer to wait and monitor the wound usually fit temporary filler into the drilled hole to keep out bacteria, food and saliva. None is better than the other and dentists make a recommendation based on their observation of the drilled hole and the state of the tooth.
Filling & Restoration
A rubber compound known as gutta percha, and a sealer paste, are the primary materials used as fillers. The exterior part of the drilled hole is sealed with a filler. The process of complete restoration is the last phase in a root canal procedure. Most often patients want a cosmetic makeover of the drilled tooth. The process usually involves the placement of a post, or crown to prevent it from breaking due to brittleness. The restoration could be occasioned by extensive decay, discolouring, or a gaping root canal hole.
Possible Complications of a Root Canal?
Root canals tend to have very high success rates in spite of the fact that it is quite an invasive procedure. Even then, sometimes root canals don’t always go according to plan. Some complications can arise during or after a root canal procedure. While some of these problems can be anticipated, many can never really be predicted. Luckily most root canal complications are rare and treatable.
Re-infection: Sometimes a root canal can fail due to a reinfection. Many reasons can lead to a reinfection. These include inadequate cleaning, exposure through a fracture, complex root formation, use of low-quality fillers and failure to remove the entire root. A trained dentist has to examine the tooth and determine whether it can be fixed or the tooth has to be removed. The remedies of the reinfection are dependent on the primary cause of the reinfection and the affected parts.
Missed Root Canals: A typical tooth has about four commonly recognised canals, which are often made of more complex canals. That’s why dentists can sometimes miss a canal in a complex tooth structure.
Crooked canals may be inaccessible during dental bleaching, and if enough bacteria are logged in there, then they may cause problems for the root canal. Accessory and lateral canals are some of the hardest to reach and clean and these missed canals can become dangerous.
Fractured Root or Crown: The removal of nerves from a tooth leaves it without any blood, oxygen or nutrient supply. This makes it brittle and fragile. Fractures on the crown or root can be detected before, during or after the root canal. Depending on the extent and severity of the fracture the dentist will advise on whether extraction or a filling is the correct option. Often fractures after root canal occur due to constant grinding, biting tough objects or lack of a crown.
Fractured Instruments: Sometimes during or before cleaning, tiny bits that chip off the dental instruments can get stuck inside a canal. This happens especially if the canal is complex and curved. A tiny bit stuck in the canal can be swallowed up into the filling during the sealing process. If it’s too big or dangerous to be left in the canal, then the dentist can use ultrasonic instruments and microscope. A larger bit can be easily removed using forceps or a scaler.
Root Canal - Frequent Asked Questions
How much does a Root Canal Cost?
The costs of root canal vary from practitioner to practitioner. Even then root canal is still one of the lengthiest and costly procedures. The cost of a root canal is usually pegged on the amount of restorative work needed to be done on the tooth. A typical root canal procedure costs between $500 and $1000 for incisors.
Root canal procedure for molars costs between $800 and $1500. An endodontist usually charges a higher cost (about 50% more) since it’s more delicate and invasive.
What is the Duration and Severity of Root Canal?
Root canal procedures are usually done in three to four stages each lasting between 30 to 90 minutes. The stages can be spaced out to within 14 days between nerve removal, fitting of temporary filler and the final sealing. The tooth infection is what causes most of the pain.
Exposed nerves tend to hurt a lot especially when they come into contact with very cold or hot foods and beverages. During the root canal procedure, the medic uses anaesthesia to make the tooth and the surrounding area numb.
Why A Root Canal Treatment?
A root canal is the most comprehensive dental procedure short of an extraction. Even then, it's painless and very beneficial for a patient with severely damaged tooth and exposed nerves. First root canal alleviates pain and discomfort that comes with exposed nerves.
Secondly, it prevents the spread of disease by eliminating the infected and diseased nerves. Thirdly it’s a restorative process that increases the lifespan of a tooth. Its restores the biting capacity and chewing sensation to a severely damaged tooth. Lastly root canal ensures that you don’t have to lose your broken teeth to extraction.
Side Effects of Root Canal Treatment?
One of the side effects of a root canal is the possibility of reinfection. This could be caused by inadequate cleaning or bacteria. There are an estimated 28 bacteria that tend to accumulate on a tooth after a root canal procedure. The most common side effects are the pain, which tends to wear off. There is also possibility of gum infection that can’t be detected by the x-rays. The most persistent challenge when it comes to root canal procedure is the trauma that comes with nerve removal. Teeth are living tissue, and the nerve removal does exert a significant level of trauma onto the tooth.
The Major Risks Associated With Root Canal?
The primary risk is that the degree of decay in some of the canals may go undetected. This will surface later on, as continued decay and weakening of the tooth. Most risks fall under misdiagonisation and inadequate treatment. The debris that occurs during drilling can also remain lodged within the root and lead to future pain and discomfort. Poorly done filling and sealing can cause the filler to drop off after sometime-though this is rare. A root canal involves taking away the nourishing ability of a tooth and this leaves it more fragile and brittle.
How Long Does Recovery Take?
The recovery of dental function after a root canal procedure lasts between a few days and a few weeks. A dull pain and inflammation may occur within the first few days after the procedure, but it soon goes away. However, it does take time before one can go back to eating hard foods. Most of the discomfort can be treated with over the counter painkillers. If the pain is sharp and persistent, then you might have to go back to the hospital for a more comprehensive assessment by your dentist.
Are There Alternatives to Root Canal?
Most often root canal is recommended for badly decayed or damaged teeth. This, therefore, means that the only viable alternative to a root canal is an extraction of the teeth.
Unfortunately, removal of teeth can affect the adjacent teeth and leave you with an uncomfortable bite. Teeth extraction is, of course, cheaper. However, it can leave unsightly gaps in the mouth and push you to opt for dental implants, which are expensive. The easier choice is to choose to keep your teeth if possible.
Trends in Root Canal Treatment
The technology and techniques around root canal have grown significantly over the past 50 years. First, the clogging of root canal used to be a persistent problem. These days it possible to clean and enlarged the drilled hole with a single tool. Secondly, there are dental instruments in the market that make it possible to access narrow, curved and complex canals. Most of these tools are disposable which helps a lot when it comes to hygiene.
Root Canal Video
Last Updated: 13 August, 2018


