Periodontal is the area around the tooth, whereas Periodontitis, simply stated, is a common gum disease. Periodontitis (pyorrhea) is as result of multiplication of bacteria in the mouth. If this condition is left unattended then periodontal disease, in its extremity, means loss of your teeth.
An extreme condition such as loss of teeth is mostly due to neglect or poor dental hygiene. Untreated, this disease is capable of affecting approximately 90% of the world population. Periodontal disease is sometimes hereditary, but it also develops in "cultured” environments, for instance, lack of proper oral dental care.
What is the Difference Between Gingivitis and Periodontitis?
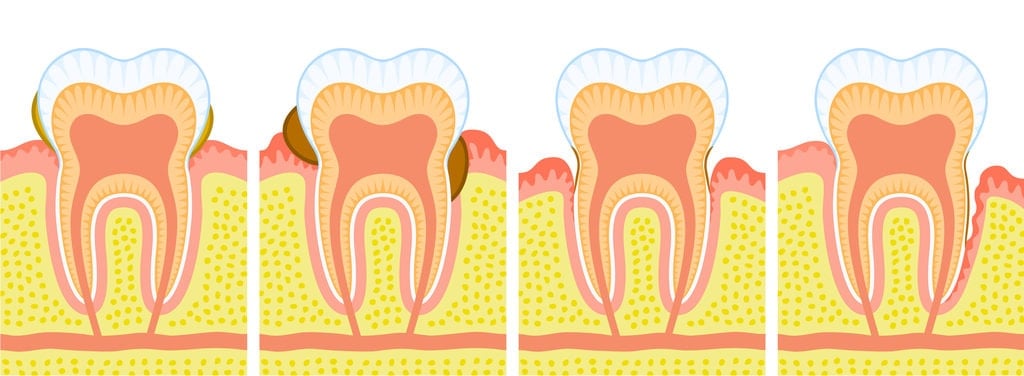
Gingivitis, in its initial stages, is characterized by red, swollen gums (inflammation) and bleeding gum occasioned by brushing your teeth. Aside from this, you may notice a build up of a discoloured layer of bacteria.
Gingivitis doesn’t always culminate into a case of Periodontitis, if it is curbed, the damage is reversible. At the onset, there is no permanent damage to the bone tissue, your teeth are still firm though your gums are suffering repairable inflammation. Removing plaque and preventing its accumulation, in most cases, cures Gingivitis.
Periodontitis is an advanced stage of Gingivitis. The gums are diseased and pull away from the teeth, the bone tissue is damaged and fragile. Studies by the American Dental Association reveal that there are about 700 species of bacteria, which live harmoniously in your mouth and the condition is normal.
The bacteria in the discussion are part of your dental makeup. However, when they multiply and are not totally dislodged, then dental problems occur. The result of this bacterial built up and the formation of plaque gives room for a healthy breeding ground for toxins.
Moreover, the toxic accumulation is because of failure of the natural bodies defence mechanism that fights the harmful bacteria. Thus, the bone tissue reduces as the battle ensues, causing the gums to pull away from the teeth forming “pockets.” These are spaces created between your gum line and teeth as the gums detatch from the teeth.
As this condition progresses, your mouth is vulnerable to infections because of the open plaque ‘pockets’. Largely, as the buid up reaches unprecedented levels, your teeth lose their support structure and shift about, creating an environment that enhances the disease because of increased “pocket” size. Periodontal disease is one of the greatest reasons for the loss of teeth in adults.
How Can I Tell If I Have Gum Disease?
Gum disease is progressive; the symptoms are subtle, thus not readily detectable. That’s the reason why a trained eye and skill of a dentist or periodontist is useful. Nevertheless, there are tell-tale signs and symptoms that you may notice. They include:
Bad breath
Halitosis, which is a word for bad breath, this smell streams from the blood and is enhanced by poor oral dental home care.
One giveaway of Halitosis is persistent bad taste and odour in your mouth, regardless of whether you brush your teeth or not. Another good indicator is also a difference in your bite, the teeth change in the way they ‘sit’ together. Authorities on the subject say that combination of the above results in bad breath and in most cases is highly accurate in the diagnosis of gum disease.
Bleeding gums
Often this occurs when you are brushing your teeth or flossing and you will notice small amount of bleeding.
Pus between the gums and teeth
Loosening of teeth and development of spaces between the teeth and gums were clearly visible.
Receding gums
Small pockets where your gums are receding from the teeth, exposing the roots in the gum. In extreme cases, teeth end up appearring longer than their regular length. The “naked” roots result in heightened sensitivity when you take hot or cold fluids or foods, which is also a characteristic of Gingivitis.
Periodontal pockets
Since the above are not always obvious, they are usually detectable only by a dentist or periodontist. However, gums will be tender, as the body’s immune system fights the bacteria build up. Most importantly, periodontal disease is chronic, subtle and doesn’t give advance warnings as your gum and bone tissue wears away. That’s why regular dental checkups are not stressed enough.
What Are The Known Causes Periodontal Disease?
The most popular causes of periodontal disease are environmental and genetic. Here is a list of the commonly known causes:
Genes
Genetic formation plays a role in periodontal disease; you can be genetically predisposed to this condition. Research shows that those with this background can be six times more likely to develop the disease. However, early intervention can keep the oral cavity clean and healthy and prevent the disease.
Poor oral hygiene
Ignoring or poorly maintained dental hygiene causes tartar accumulation, a combination of this and lack of professional dental care will lead to disease.
Menopause and pregnancy
You may not be aware but your body undergoes hormonal changes in menopause or pregnancy so calls for a clear understanding and participative action. You need to floss and brush your teeth regularly and appropriately, the disease is multifactorial, this is one way to reduce its risk and halt its progression.
Medical conditions
Diabetics, Pulmonary, and Cardiovascular disease are closely associated with periodontal disease. However, research reveal that the causal relations are yet to be fully established, but there is a definite correlation.
For instance, Diabetes inhibits the body’s capability to use insulin, thus encouraging bacteria growth that in turn is hard to cure and control. Medics maintain that there a definite relation between Diabetes Type 1 and periodontal disease.
Tobacco consumers
On the front of community dentistry, reveals that smokers and those who use tobacco increase their chances of periodontal disease. Take for instance; in the case of gum inflammation, the excessive pollutants from a cigarette elevate the progress of disease.
Furthermore, persistence in these habits frustrates the efforts of treatment. Tobacco consumers include those who use electronic cigarettes, pipes or cigars, and snuff, these are the advocates for oral cancers.
Is there Treatment or Cure for Gum Disease?
The goal of treatment, in gum disease, is to reduce the pockets caused by toxic build up and shifting teeth. Also, treatment entails smoothing the rough surfaces, eliminating plaque and calculus (tartar) around the teeth. A dentist or dental hygienist can treat gum disease using various approaches and introduced dental implants. Here are five treatments (although they are more):
- Scaling and root planning: this involves deep penetrative pocket cleaning.
- Bone grafts: adding bone tissue, usually from you, to create a platform for regrowth and stability.
- Soft Tissue Grafts: the periodontist takes tissue from your palate and uses sutures to place this where your gum is in recession.
- Prescription: the specialist can opt to prescribe antibiotics, antifungals, and gels that help treat and stop the progress of the disease.
- Gum recontouring: If the recession of your gums ends up giving you a “toothy” smile, your periodontist can re-contour the gingival tissue. The treatment will correct and even out your smile.
Unfortunately, Periodontitis is irreversible as the support structure of the bone and tissue is already destroyed and irreparable. In extreme cases, the patient develops elongated teeth and permanently receded gums causing disfigurement. However, constructive and plastic surgeries are the corrective measure in such situations.
Is There Preventive Measure Against Gum Disease?
Like with most circumstances, prevention is better than a cure to avoid dire consequences. It is good practice to maintain hygienic oral home care and to seek professional advice. Here are some ways to prevent gum disease:
Dental visits
Make due diligence to see your dentist at least twice annually to ascertain everything is in order. Your dentist is able to detect and curb gum disease before it develops and destroys your teeth and gums.
A dentist is able to tell you what may have caused the condition in the first place. Thus, armed with such information you are in a better position to stop a habit or activity if it is a contributing factor.
In addition, a professional carries out the necessary cleaning, exams, and x-rays that help preserve the natural teeth and proper support structures if need be.
Your dentist is skilled and trained to help halt the onset, progress, and repeated occurrence of periodontal disease.
Oral home care
Brush your teeth, properly, use a toothbrush structure to reach the not so easy to reach areas. Also, floss regularly, this dislodges the notorious plaque and leaves no room for bacteria growth. Flossing cleans the spaces between your teeth that are hard to manipulate using a toothbrush.
Healthy nutrition
Eating healthily boosts your immune system and lowers chances of infection. Medical studies show your Calcium and Vitamin D intake improves your bone density preventing osteoporosis, makes for better dentition, and tooth retention.
Comfortable bite
You may be in the habit of grinding or clenching your teeth, this upsets your natural bite. Persistence leads to tension build up in your oral area and threat of rupturing the supporting tissues around your teeth.
Periodontal disease is avoidable, practicing hygienic oral dental home care and professional check-ups are good measures to adopt. In instances where you are genetically predisposed to the condition, early interventions are mandatory to prevent disease development to dire situations.
If it is too late and the disease has advanced, some measures can retard and stop the progress of the disease.
Living a healthy lifestyle, such as avoid smoking, eating healthy, flossing and brushing your teeth regularly go a long way to help prevent periodontal disease, be vigilant.
Remember that your teeth are not only essential for chewing and enhancing your smile, but they are also part of your overall beauty, hence the need to be in good shape.


